
Cannabis & The Gut: Does Weed Heal Or Harm?
Does cannabis quell nervous stomach? Does the herb really cause some people to vomit a lot? How does cannabis impact the gut, anyway? Here are the answers.
Many people turn to cannabis as their go-to relief from an upset stomach or gastrointestinal distress. There is ample evidence out there that the herb can quell some of the worst cases of nausea, spark your appetite, and calm your bowels. Yet, sadly to say, recent research shows that there may be some less than desirable digestive effects for some chronic consumers. For a rundown of the good and the bad, here’s how cannabis affects the gut.
What is the endocannabinoid system?
To better understand how cannabis impacts the gut, it’s helpful to know a little about how the herb engages the body. The active compounds in cannabis interact with cells in the body through the endocannabinoid system (ECS).
The ECS is a large communication network in the body. It is made up of cell receptors, chemical compounds, and the enzymes that make the chemical compounds.
The cell receptors are called cannabinoid receptors, and thus far, there are two of them: CB1 and CB2. The chemical compounds are called endocannabinoids. Endocannabinoids are the body’s natural THC. In fact, they were named after the active components of cannabis, called phytocannabinoids.
The ECS has many functions in the body. In fact, it’s primary responsibility is to promote homeostasis, which means optimum balance. This includes regulation of mood, mobility, pain, immune function, metabolism, sleep, and reproduction.
For a simple yet detailed explanation of the ECS, check out the full article here.
The ECS and the gut
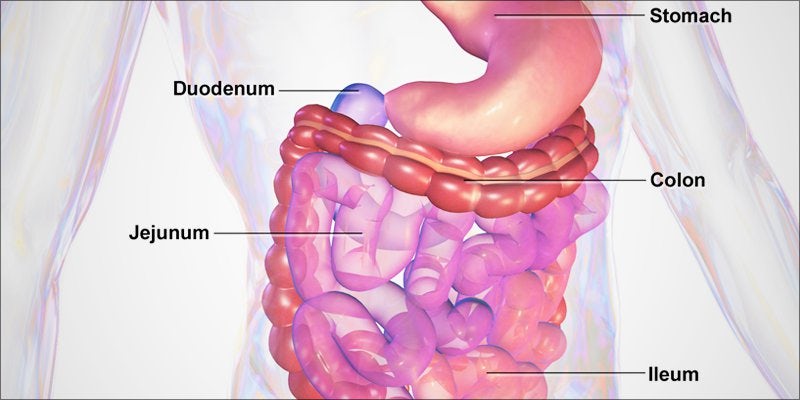
In a way, the ECS is sort of like an orchestra conductor. It makes up the signal messages that trigger all sorts of biochemical interactions. Many of these interactions occur between the brain, the immune system, and the gut.
The gastrointestinal (GI) tract houses 80% of the immune system. GI tract also contains cannabinoid receptors. Research has shown that high levels of endocannabinoids are found throughout the digestive system.
Research is still lacking on the exact function of endocannabinoids in the gut. Yet, the ECS seems to play many roles in the GI tract. These include,
- Regulation of stomach acid
- Motility (ability to move food from the mouth and out again as a bowel movement)
- Visceral sensation (ability to perceive bodily organs)
- Inflammation (immune response)
- Pain
- Satiety (feeling full)
Both the CB1 receptor and the CB2 receptor can be found in the gut. The CB1 receptor is the cell site responsible for the high caused by psychoactive THC. Though most abundant in the central nervous system, the CB1 receptor is expressed on nerves that connect the gut to the brain.
The CB2 receptor is a bit tricky. In a healthy gut, a 2008 review suggests that CB2 receptors are not very abundant. But, when the GI tract is inflamed and in the case of bowel diseases, levels of the CB2 receptor increase. The CB2 receptor is most common on immune cells.
The fact that CB2 receptors are increased in damaged or sickly intestines is a good sign that cannabinoid therapy may be useful in gastrointestinal disease. GI diseases are discussed in more detail below.
Gut-brain axis

Another fascinating way the ECS engages the gut is through the gut-brain axis. In the Victorian era, it wasn’t uncommon to hear the phrase “I have bowels for you” as an expression of empathy. Today, idioms like “gut feelings” and “butterflies in the stomach” are still popular. There’s a reason this language exists. The gut and the brain are intimately connected.
One way that they are connected is through the ECS. A 2016 review published in Gastroenterology found that the CB1 receptors control the body’s visceral sensation. “Visceral sensation” is the response and perception of the internal organs. Of course, this includes the gut.
Turns out, the gut and the brain communicate with each other through what is called the “gut-brain axis”. This is a series of nerve connections and chemical signals that help the two major organ systems coordinate and send messages to each other. They are so intimately connected that recently the gut has been called “the second brain”.
When one part of the body is under stress, whether from signals from the central nervous system or signals from the gut, the other responds with vigor. The ability to feel this response partly depends on the ECS. The ECS links stress to visceral pain and GI function.
Those who’ve experienced nervous stomach or have suddenly needed to run to the bathroom after a stressful event have likely experienced the connection between the ESC, gut, and brain first hand.
How does cannabis affect the gut?

The ECS is what allows cannabis to have an effect on the body. THC activates both endocannabinoid receptors. This may explain why many with nausea and GI distress find strong relief with cannabis.
Yet, the effects of the herb largely depend on what you’ve got going on in the first place. In some people, the impacts of cannabis may be highly desirable. Cancer, IBS, and wasting disease are great examples. In others, too much cannabis may have negative impacts. Here’s why,
THC may reduce stomach acid
Have acid reflux? What about heartburn? It’s important to pay attention to whether or not cannabis makes this condition better or worse. Popular belief has it that acid reflux and heartburn are caused by high levels of stomach acid. If this is the case, then there is evidence that cannabis may help.
However, some experts suggest that low stomach acid and too much abdominal pressure may actually be the underlying issue. With low stomach acid, it’s possible that cannabis may aggravate the issue.
Here’s how cannabis is involved: the CB1 receptor tells the stomach to stop producing stomach acid. In some cases, this may be beneficial. However, if digestive problems are caused by low stomach acid, THC may not actually help.
An early study published in the 1970s found that consuming cannabis more than twice a week was associated with low stomach acid. This is potentially good news for those with peptic ulcers, yet the news isn’t so great for those who have the opposite problem.
Low stomach acid (Hypochlorhydria) means that food may not be digested properly. Some signs of low stomach acid include:
- Anemia
- Heartburn
- Bloating and gas after meals
- Indigestion
- Nausea
- Carbohydrate malabsorption
There is not enough research to discuss the potential impacts of cannabis on stomach acid. It is also unclear whether tolerance to THC has an impact on gastric acids. To better understand these effects, this study sorely needs to be replicated.
Fun fact: many people take supplements like Betaine HCl and digestive enzymes to improve their stomach acid, though it’s best to work with a doctor before taking any new supplement.
Some people have increased nausea with cannabis

It’s well-known that cannabis can ease stomach pain and reduce nausea and vomiting. Many even feel that they have no appetite or are unable to digest or process food without the help of cannabis. Cancer and HIV/AIDS patients with medical recommendations often experience this firsthand.
However, in some cases, chronic cannabis consumption may increase nausea and vomiting. Lately, there has been talk of a rare condition known as “cannabinoid hyperemesis syndrome”. There is very little research on the topic minus case reports.
Cannabinoid hyperemesis syndrome (CHS)
Not much is known about this condition, but for some reason, after a period of heavy and prolonged cannabis use, some people have experienced intense cyclic vomiting and nausea. Those with this condition also tend to compulsively bathe in hot water.
A 2011 study from Temple University found that most case studies of CHS are young adults. CHS symptoms began after three years of chronic cannabis consumption. Daily use is reported, often more than three to five times a day.
The study articulates that cannabis is normally an antiemetic (anti-vomiting) agent, but for some reason things go awry. Some possible reasons for this include,
- Low stomach acid
- Slowed digestion and bowel movements
- Relaxed lower esophageal sphincter (the valve that connects your stomach from your esophagus)
- Increased visceral sensitivity and pain
- Increased inflammation
Basically, theory has it that a relaxed lower esophageal sphincter makes it easier to vomit. Low stomach acid means that there’s probably some undigested food in the gut. THC also can slow down bowel movements, creating a buildup of nasty stuff in the digestive tract. All of these things together trigger the body to vomit. Hot showers provide temporary relief.
The anti-nausea and vomiting effects of cannabis are largely attributed to the herb’s impact on the central nervous system. But, this review suggests that cannabis may have the opposite effect in the gut.
So, the authors suggest that the overall impact of the plant on digestion is paradoxical. The gut says “vomit”, and the brain says “don’t”. Looks like the gut wins in this case.
Is CHS even real?
CHS is very new in terms of medical recognition. Minus some case studies and a few reports, there is a lot left to be desired in terms of substantial research. However, it’s important to note that when it comes to cannabis science, things are extremely complex.
One feasibility study, for example, has shown that cannabis treatments may improve constipation in patients undergoing methadone treatment.
Cannabis can also be one heck of a nausea-fighting herb. Research has found that activating the CB1 receptor calms down nausea and reduces vomiting. On the contrary, blocking CB1 receptors triggers vomiting. Cannabis activates, not blocks.
There is also no mention of what percentage of people may have this response.
Further, many other diet and lifestyle factors also contribute to low stomach acid and constipation. So, it is difficult to tell whether or not it is the cannabis itself, or whether it is a perfect storm of conditions that contribute to cannabinoid toxicity.
All in all, everybody is different. Not everyone develops CHS. As one critique suggests, people have been using the herb for thousands of years without noticing this issue. There isn’t enough information to know whether some people are genetically predisposed or if certain environmental factors amplify the condition.
Concerned about this? Periodic tolerance breaks seem like they may help.
Can cannabis help gastric diseases?
With potential negatives out of the way, let’s get to the good stuff. The anti-inflammatory and pain-fighting properties of cannabis may be highly beneficial for those with certain digestive diseases. In fact, many researchers have argued for more studies on cannabinoids for gastrointestinal disorders.
Here are three conditions with promising research:
1. Celiac disease

Research shows that cannabinoid receptors can heal damage to the intestinal lining in diseases like diverticulitis and celiac disease. In a 2010 review, researchers explained that certain endocannabinoids are more abundant in the small intestines of those with celiac.
Another 2005 study found that CB2 receptors were over-expressed in mucous membranes (epithelial cells) of the colon. CB2 receptors play a part in the immune system. Activating these receptors with cannabinoid therapy may calm down gut inflammation and heal damaged tissue.
In celiac disease, the immune system begins to wage a war on the epithelial cells of the small intestine. The findings that cannabinoids promote epithelial healing is quite promising. THC directly engages the CB2 receptor. CBD indirectly affects the cell site.
For more information on cannabis and celiac disease, check out our full article here.
2. Irritable bowel syndrome
No one knows the exact cause of irritable bowel syndrome (IBS), but inflammation in the gut plays a big part in the condition. IBS can cause either diarrhea, constipation, or both. Those with diarrhea may benefit from THC’s ability to slow things down.
In fact, one 2005 study found that the herb did just that. Cannabis reduces intestinal mobility and can reduce intestinal spasms in those with IBS. Further, pain and visceral (organ) perception are heightened among those with IBS. Some suggest the endocannabinoid system may be partly responsible.
Some researchers suggest that irritable bowel syndrome (IBS) is attributed to an endocannabinoid deficiency. This means that, for some reason, the body does not produce enough endocannabinoids. In turn, this causes issues with inflammation and digestive troubles.
A review published this year [2016] in Gastroenterology has found that mutations in genes responsible for coding the CB1 receptor are linked to some types of irritable bowel syndrome. As mentioned earlier, CB1 receptors help regulate inflammatory response and motility in the gut.
3. Crohn’s Disease
Crohn’s disease garners a medical cannabis authorization in many states. For good reason, too. Intense pain, severe intestinal inflammation, ulcers, and endless trips to the bathroom can make life absolutely miserable.
Not only is there a wealth of anecdotal information on cannabis for Crohn’s disease, but a few human trials have had positive results.
In a small, placebo-controlled study conducted in 2013, almost half of all cannabis-treated patients achieved complete remission. 5 out of 11 patients had unbelievable success with smoked cannabis for Crohn’s disease. 10 out of the 11 showed a clinical response to the herb.
Another observational study had similar results. 30 cannabis-consuming patients had improved their quality of life and reduced symptoms in Crohn’s. The patients had a reduced need for surgery after beginning cannabis treatments. Many were also able to reduce the use of prescription medications.
For more information on cannabis for Crohn’s disease, check out the full article here.
The relationship between cannabis and the gut is complex. There is a lot more going on in the digestive tract than most care to admit. This brief article skims the surface of the intricate interactions between cannabis and the intestines.
A lack of research still leaves a lot in the dark. Further, this article does not mention the detailed relationship between the ECS, our digestive system, and the trillions of microbes that live in our gut.
All in all, the GI tract is like the wild west of the body. Only with time will science reveal more about this complex system.
Herb Recommended Products:
READ MORE










